Although vision is not the leading sense in dogs and cats, which orient themselves primarily through a perfect sense of smell and hearing, it is undoubtedly essential for proper functioning and comfort. Cataract plays a special role among the causes of blindness due to its high incidence.
If your dog is diagnosed with the onset of cataracts or you are a veterinarian who encounters vision problems in your patients on a daily basis, be sure to read the article below by the veterinarian Paweł Stefanowicz, a specialist in the field of veterinary ophthalmology, who introduces the genesis, symptoms, methods of diagnosis and treatment, as well as postoperative procedures related to cataract removal in dogs.
FUNCTIONS AND CONSTRUCTION OF THE EYE
To discuss the issues and better understand what cataracts are, we should start from scratch in order to get to know the structure of the eye and understand its functioning.
Like humans, dogs have eyelids that are responsible for protecting the eyeball. However, they also have an additional eyelid (third eyelid) located in the paranasal corner. The third eyelid, due to the participation in the production of the tear film and the ability to cover the eyeball, not only protects the eye, but also has a cleansing function. Equally important tissue is the eyelid and ocular conjunctiva, i.e., the mucosa that forms the conjunctival sac, which is an important element of the eye supporting apparatus. Another important morphotic structure is the pre-corneal tear film, which ensures adequate hydration of the eye. Further anatomical elements of the eyeball can be divided into anterior and posterior segments.
The anterior segment of the eye includes the cornea, the anterior sclera, an anterior chamber filled with intraocular fluid, the iris, the posterior chamber, and the lens. There is also a drainage angle (iris-corneal angle) in the front of the eye, which is responsible for filtration, i.e., drainage of intraocular fluid.
In the posterior segment of the eye, behind the lens, is the vitreous body. It is a large, gel structure that fills and stabilizes the inside of the eyeball, while allowing the proper adhesion of the retina to the uveal membrane. The next elements are the posterior uvea, the posterior sclera (a structure that is part of the fibrous wall), the retina and optic disc, and the optic nerve itself, which conducts impulses from the retina to the central nervous system.
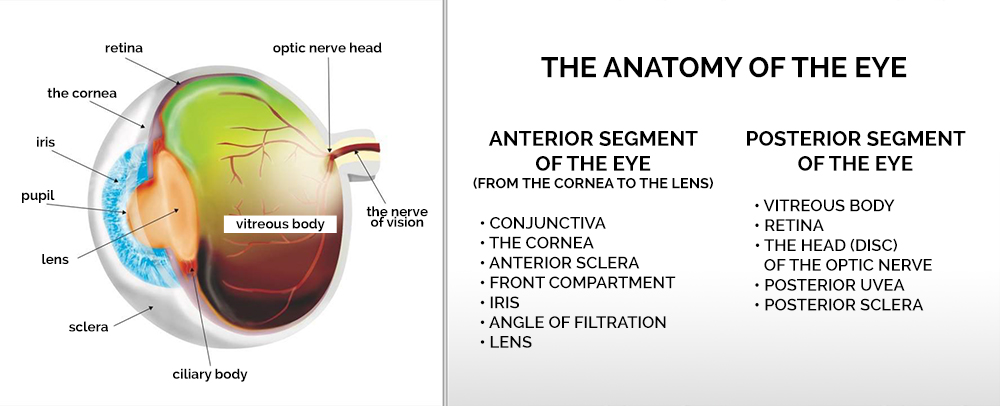
Simply put, the function of the eyeball consists in taking light into the eye, focusing it on the photosensitive retina, and then processing it into an electrical impulse that is transmitted to the central nervous system where visual impressions will arise. For this reason, the eye structures that are elements of the so-called visual pathway – including: the cornea, intraocular fluid and the lens must be perfectly transparent and fully transmissive to light.
CATARACT – LENS DISEASE
Cataract is a disease that affects the lens of the eyeball, which is a transparent, flexible, non-vascular and innervated organ located in the anterior segment of the eye. The lack of vascularization and innervation of the lens is due to the fact that any blood vessels and nerve endings would interfere with the transparency of the lens, which is necessary for proper vision. The 360 ° lens hangs on the muscles and ligaments of the ciliary crown that attach it to the ciliary body. The lens has an anterior pole, a posterior pole, and an equator. Interestingly, it is not perfectly symmetrical, but its rear curvature is slightly greater.

The lens, while appearing to be an amorphous, crystal-clear structure, is a tissue and like any other tissue, it is made of cells. It is covered with an anterior pouch with an anterior epithelium inside and a posterior pouch with a posterior epithelium underneath. There are also lenticular fibers, the arrangement of which can be compared to the arrangement of layers in an onion, and the fibers lying on top of each other form the nucleus and the lenticular cortex. The lens also has seams which take the shape of the letter Y for the front part and the shape of an inverted Y for the back part.
The primary role of the lens is accommodation. The lens changes its shape, focusing the light rays at the right angle on the back of the eye, on the retina. The focused light stimulates the photoreceptors and creates an impulse that is then transmitted to the central nervous system. The image created in this way is inverted and reduced. In the case of dogs and cats, the accommodative function of the lens is not as important as it is for humans. The same role is played by other elements of the eye, which include: a large, convex, strongly arched cornea and a very deep, fluid-filled posterior chamber of the eye.
SPECIAL FEATURES OF THE LENS AND ITS METABOLISM
To visualize how delicate the structure of the lens is, it is enough to compare the thickness of its posterior capsule (4 microns) to the thickness of the red blood cell (7 microns). It is easy to imagine how precise the cataract surgery on a dog must be and how careful the surgeon must be to avoid simultaneous damage to the eye lens.
As mentioned earlier, the lens is innervated and vascularized. Meanwhile, every living tissue must absorb nutrients and donate metabolites, which is most often done through blood and blood vessels. So, what does the lens allow us to see? In this case, the functions of the blood vessels are performed by the intraocular fluid, produced by the ciliary body, which supplies the lens with nutrients, e.g., carbohydrates, extremely important for glucose management and, at the same time, for the condition of the eye lens. The lens is characterized by an active metabolism. Its cells are produced throughout life, and therefore there are more and more fibers, which is important for thickening its structure.
The composition of the intraocular fluid that nourishes the lens changes during various metabolic and intoxicating diseases and inflammatory processes taking place in the vascular membrane of the eye. The energy demand of the lens is met by glucose metabolism, broken down in anaerobic processes with the participation of hexokinase or in the aerobic process in the citric acid cycle.
Diabetes mellitus, which we know is a serious metabolic disease, disturbs the carbohydrate metabolism, causes the formation of a significant amount of sorbitol and the deposition of carbohydrate substances in the lens. Carbohydrate retention is combined with water retention, which causes swelling and clouding (diabetic cataract).

A healthy lens consists of about 35% of proteins. With age and because of systemic and extra-systemic diseases, the protein character in the lens changes, in which the insoluble proteins take the advantage over the soluble ones.
NUCLEOSCLEROSIS – OLD SCLEROSIS OF THE NUCLEAR LENS
With age, as in humans, apart from cataract changes, there is also the so-called senile nucleosclerosis. This is the result of increasing cell production, water loss and a change in the protein composition of the lens, which strongly thickens its nucleus. However, sclerosis, or the hardening of the lens nucleus, is not yet a cataract. It slightly disturbs accommodation and does not clearly impair vision. It should be emphasized that in dogs and cats’ vision is not the leading sense and sometimes even serious problems with transparency in the visual track do not cause significant disturbances in their functioning.
FACTORS FOR THE FORMATION, DEFINITION AND CLASSIFICATION OF CATARIS
Although the lens is originally 65% water, which is less than most other tissues in the body, it becomes more dehydrated with age. There is less and less water and more and more cells in the lens. Its protein structure also changes with age. All this causes unfavorable changes in it, from nucleosclerosis to cataracts. The very process of cataract formation in a dog is therefore evidence of the multifactorial nature of this disease. In her case, there is no one type of pathogenesis, one reason for which it arises. However, there are factors that largely contribute to its occurrence. A cataract is defined as blemishes or clouding of the lens that make it difficult for light to enter the retina, and consequently cause visual impairment. The larger the endosperm on the dog’s eye, the greater the deterioration in visual acuity.
In the case of quadrupeds, we can talk about breeds in which the genetic condition increases the risk of cataracts. They include, among others Afghan hart, Boston Terrier, or German Shepherd Dog, which in recent years, as a result of the breeding process, has significantly worsened ophthalmological problems. Cataracts are also more common in golden retrievers, labradors, and poodles than in other breeds.

Cataracts in a dog are classified according to its degree and time of origin. In this case, we can distinguish congenital (hereditary) or secondary (acquired) cataracts. We can also describe it in terms of the cause. We distinguish between primary and secondary cataracts.
Congenital cataracts can be triggered by accompanying developmental defects not only related to the lens itself. Such defects include persistent hyperplastic primary vitreous (PHPV), persistent pupillary membrane (PPM), small eyes, retinopathy, retinal detachment, and uveitis. Because dogs and cats may have such malformations, it is recommended to perform tests for the presence of hereditary defects. Performing such a test allows, among others conducting animal husbandry that is conscientious and safe for the health of animals.

The triggers of congenital cataracts are also those that influence embryonic development. These include intrauterine infections and maternal metabolic disorders, as well as physical factors such as ionizing radiation and certain medications (sulfonamides, corticosteroids).
The dog may also develop secondary cataracts as a concomitant disease, incl. diabetes mellitus, uveitis, keratitis and scleritis, eyeball injuries, neoplastic lesions, congenital retinal dystrophies, glaucoma or hypothyroidism and hyperparathyroidism.
A further classification of cataracts includes the types distinguished in terms of their location. There are anterior pyramidal cataracts, capsular cataracts, anterior subcapsular cataracts, anterior cortical cataracts, nuclear cataracts, equatorial (peripheral cortical), posterior cortical, posterior subcapsular and posterior capsular cataracts. Cataracts are also classified according to their nature: focal (with lesions located only in certain places), diffuse, vacuolating and geographic (in the form of large continental-shaped spots).

DIAGNOSTICS
When diagnosing a patient, the size of all lesions on the lens should be accurately described. In the case of cataracts, we are talking about its maturation, i.e., the transition from the initial form to the immature, mature, and then super-mature form, and finally to the Morgani cataract, i.e. into the apparently disappearing cataract, in which the already opaque cortical masses begin to liquefy. At this stage, the lens becomes translucent again, but the liquefaction causes further serious ophthalmic problems such as uveitis. In the case of cataract-induced uveitis, or if it is at risk, the only solution is cataract surgery – phacoemulsification.
OFTHALMOSCOPY, USG
Ophthalmoscopy, i.e., a diagnostic examination, is performed with the use of ophthalmic tools such as eyeglass loupes, which allow you to examine the appendages of the eye and eyelids, i.e., the external ophthalmic condition, and slit lamps (hand slit lamps are used in veterinary ophthalmology). Another tool that allows you to examine the fundus is a direct or indirect ophthalmoscope equipped with appropriate lenses that focus the light on the fundus. Such an examination should be performed whenever the stage of cataract development does not impair vision sufficiently to prevent light transmission through the lens. The endosperm on the dog’s eye and the fundus can also be carried out digitally, using so-called fundus cameras. In each ophthalmic examination, as well as in preparation for cataract surgery, intraocular tonometric testing should be performed.
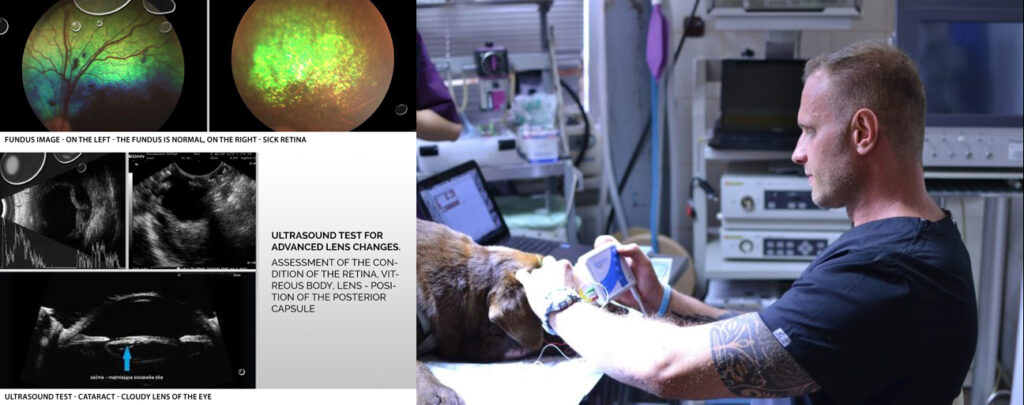
Ultrasound is also a diagnostic method that we can use in patients with cataracts. The ophthalmologist should use them when the lens is so changed that it no longer transmits light, thus making it impossible to examine the posterior segment and the fundus, i.e., the assessment of the retina and vitreous body. Ultrasound examination helps to avoid unpleasant surprises during surgery, e.g., retinal detachment. The lens in the ultrasound image should be hypoechogenic, i.e., black. Hyperechogenicity, i.e., the thickening of the structures on the lens, indicates the presence of pathological changes, including cataracts.
RETINA ELECTROPHYSIOLOGY – ERG
A dog with known cataracts and no fundus examination should undergo a neurophthalmic examination to examine reflexes such as the pupillary reflex (PLR), the dazzle response, or the menace response to the approaching object). Before cataract surgery, the doctor should also perform an ERG electrophysiological examination, which will clearly confirm the functioning or lack of function of the retina. If it is not functioning, cataract surgery does not restore the patient’s sight, which the dog owner should be informed about. The ERG test measures the activity of the retinal photoreceptors stimulated by light.
Thorough blood screening, including biochemistry and complete blood counts, should also be performed to diagnose coexisting causes or health problems that may have led to the development of cataracts. These tests should also be performed before the operation itself, as well as prepare the patient for it anaesthesiologically, i.e., check whether he or she qualifies for anesthesia. For this purpose, an echocardiographic examination (echo of the heart) should be performed.
QUALIFYING FOR CATARACT SURGERY
When assessing the possibility of cataract surgery, the patient’s age should also be considered. In older dogs, there may be motor and cognitive disorders that adversely affect the treatment. The character of the dog is also an extremely important factor, namely its ability to cooperate with the guardian and the doctor. Unfortunately, it happens that the reluctance to cooperate on the part of the animal, aggression and a tendency to self-harm preclude effective treatment after surgery and reduce the chances of a cure.
A comprehensive approach to the diagnosis of the patient is extremely important, allowing the detection of the disease at an early stage of its development, i.e., when it is possible to achieve the optimal effect of cataract treatment in a dog.
Phacoemulsification, i.e., cataract removal surgery, should be performed in the early stages of cataracts. This is when ophthalmological problems secondary to unoperated cataracts have not yet developed, and there is the lowest risk of postoperative complications. The quick qualification for the procedure should be remembered especially in the case of diabetic patients, who have an increased risk of swelling and even rupture of the lens capsule, which may lead to severe uveitis. If uveitis is present, it should be managed with appropriate treatment before surgery.
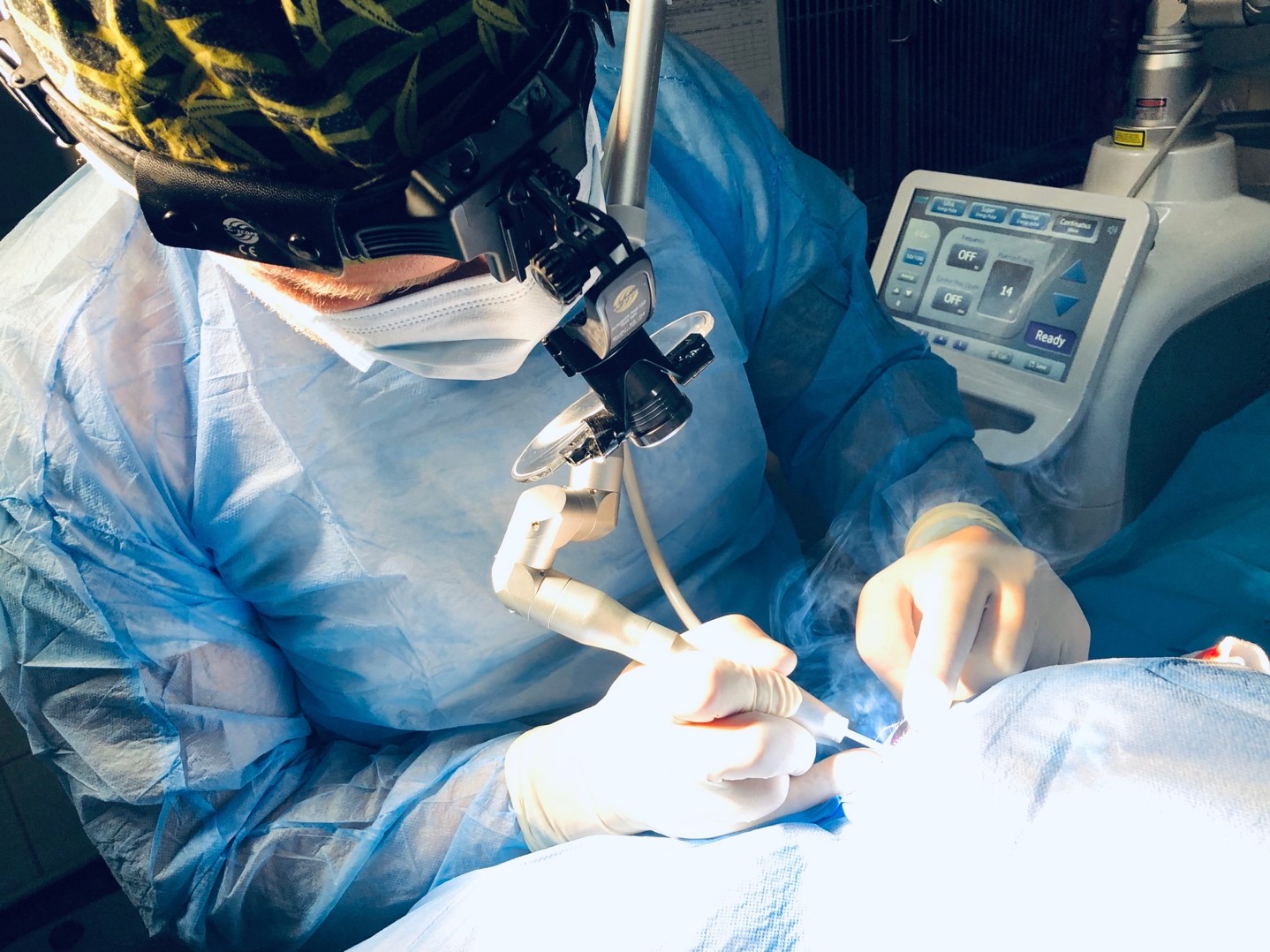
PREPARATION FOR THE TREATMENT – INSTRUMENTARY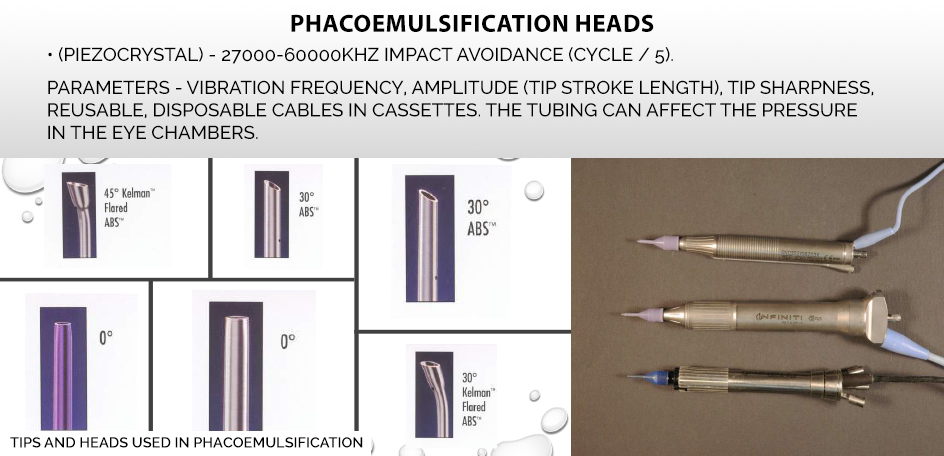
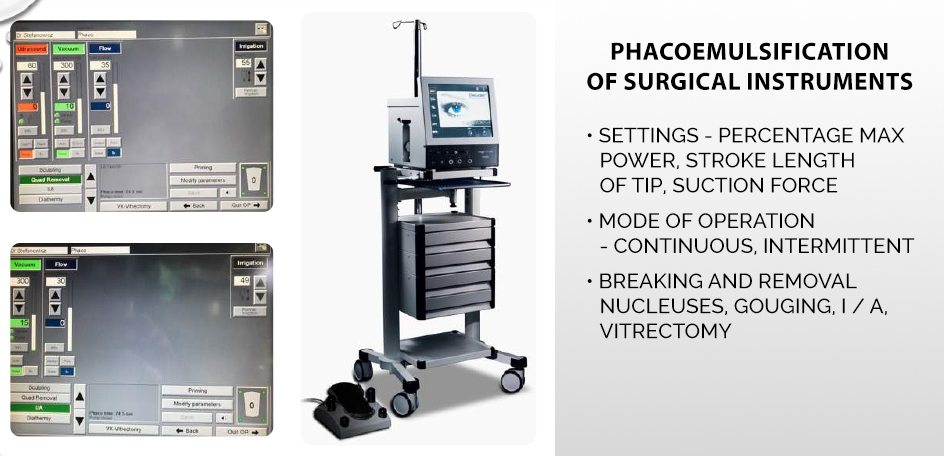
The microsurgical instruments used in cataract surgery in dogs are the same as in the case of human ophthalmology. Cataract removal procedure – phacoemulsification (Latin phacoemulssificatio cataractae), uses ultrasound vibration, and the device used to perform the operation is a phacoemulsifier equipped with a so-called tip, i.e., properly selected tips mounted on the heads, inducing ultrasounds that break and then suck out the broken cortical masses from the eye.
FHACOEMULSIFICATION – THE COURSE OF CATCHER REMOVAL
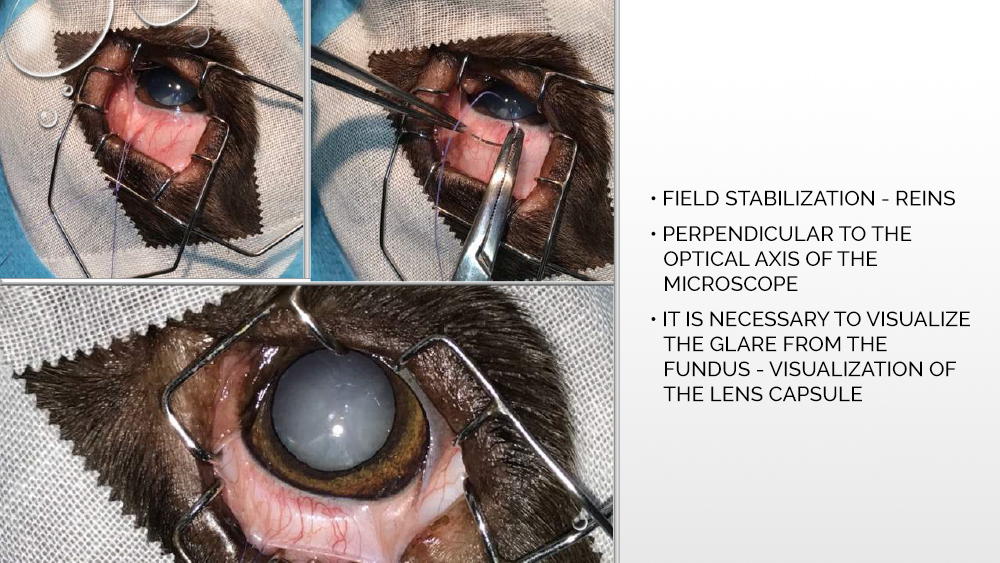
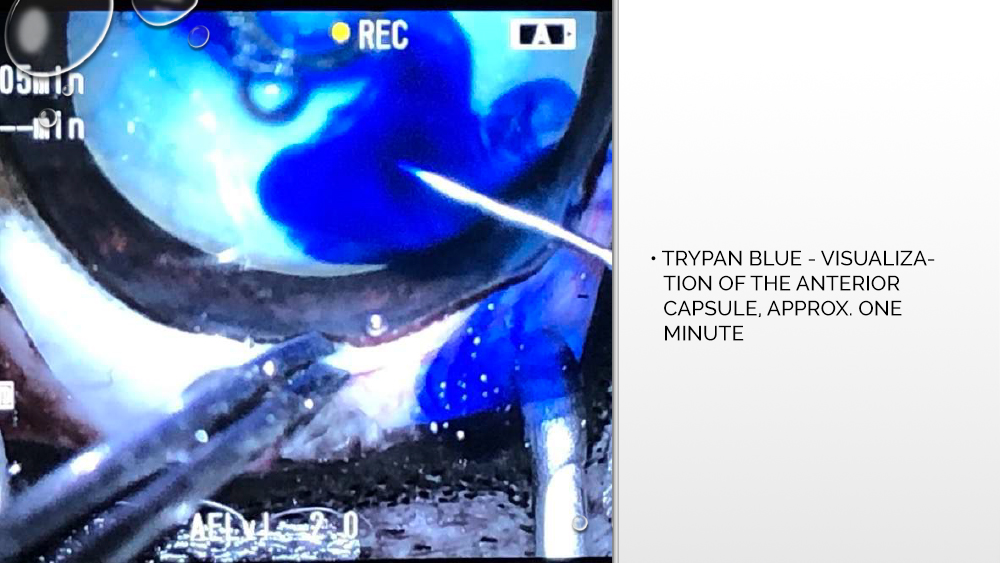
Before the phacoemulsification procedure, the patient is placed in a stable position on the back, the surgical field is disinfected, and pads are placed under the head to absorb the fluids released during the procedure. It is especially important to stabilize the eyeball in a perpendicular position to the optical axis of the microscope. Then, with a corneal knife, a corneal incision is made, opening the anterior chamber of the eyeball, into which trypan blue, a dye that allows the anterior capsule to be visualized, is administered.
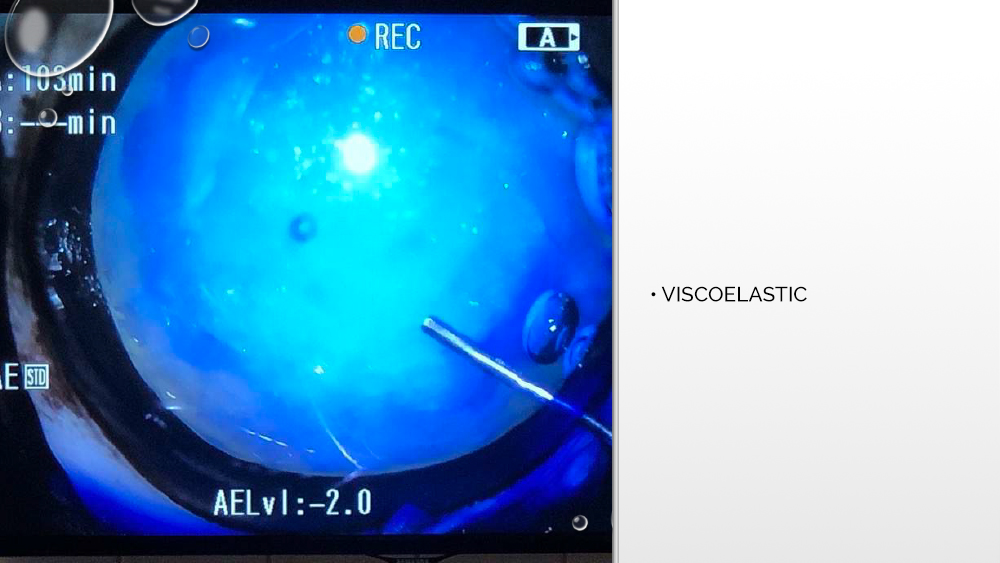
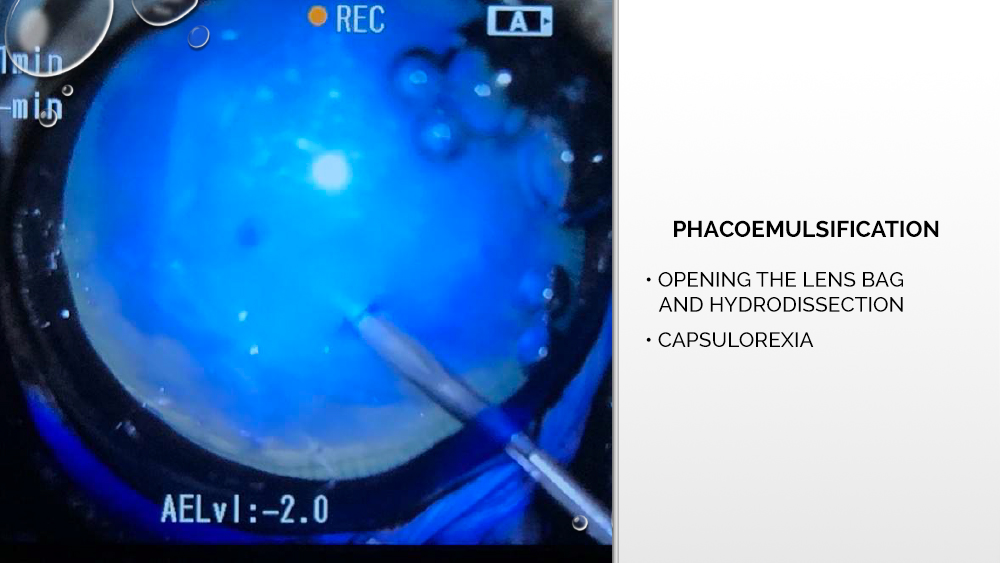
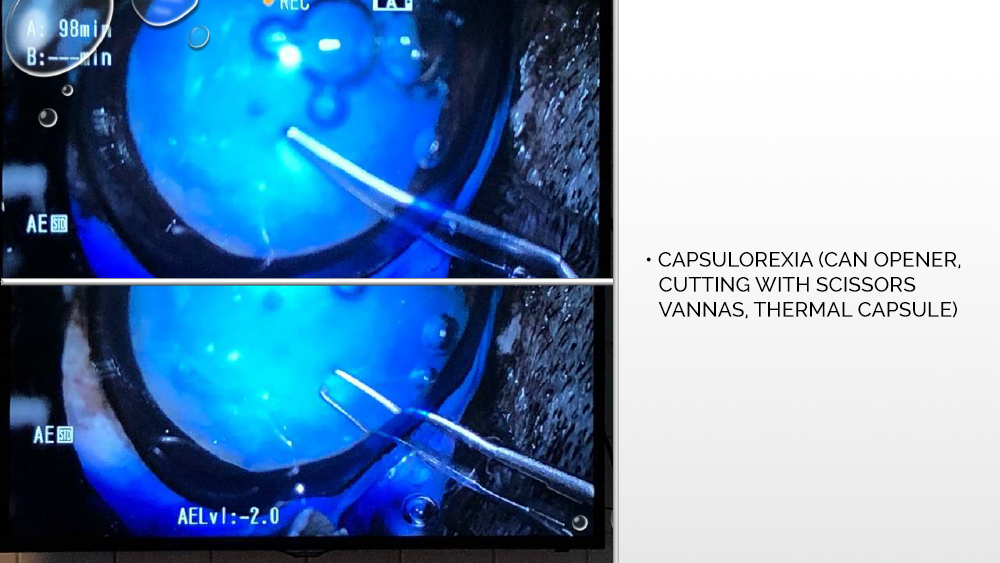
The next step is to apply a suitable viscoelastic to the inside of the eyeball, i.e., a gel that will fill the space between the lens bags and stabilize the anterior chamber of the eye. Then, further opening of the lens capsule takes place, with hydrodissection in some cases also possible, i.e., administration of a fluid that spreads under the capsule and separates the cortical masses from the lens capsule. Capsulorexia, or opening the anterior lens bag, is performed with a laser, which some phacoemulsifiers are equipped with, or with the use of a capsulotome.
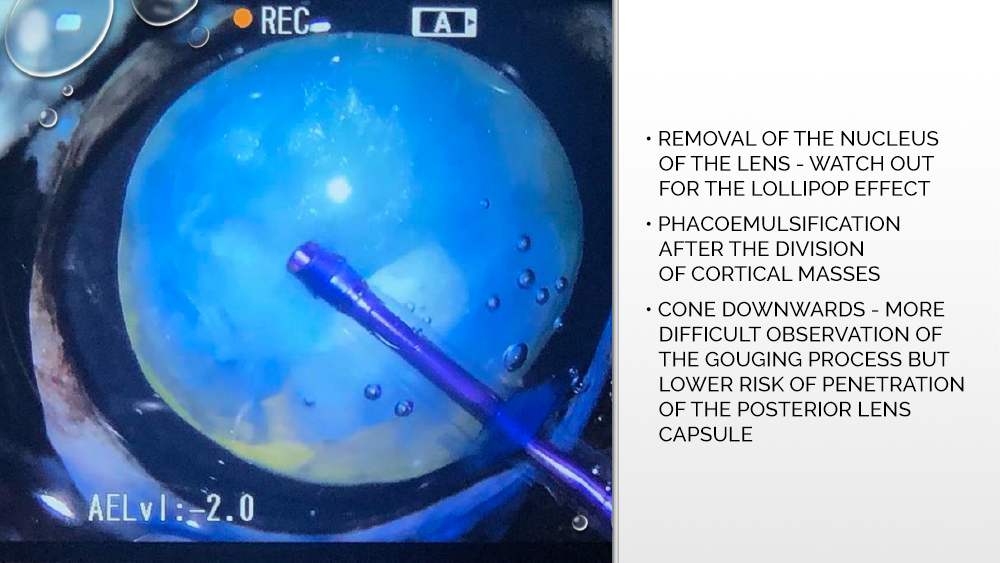
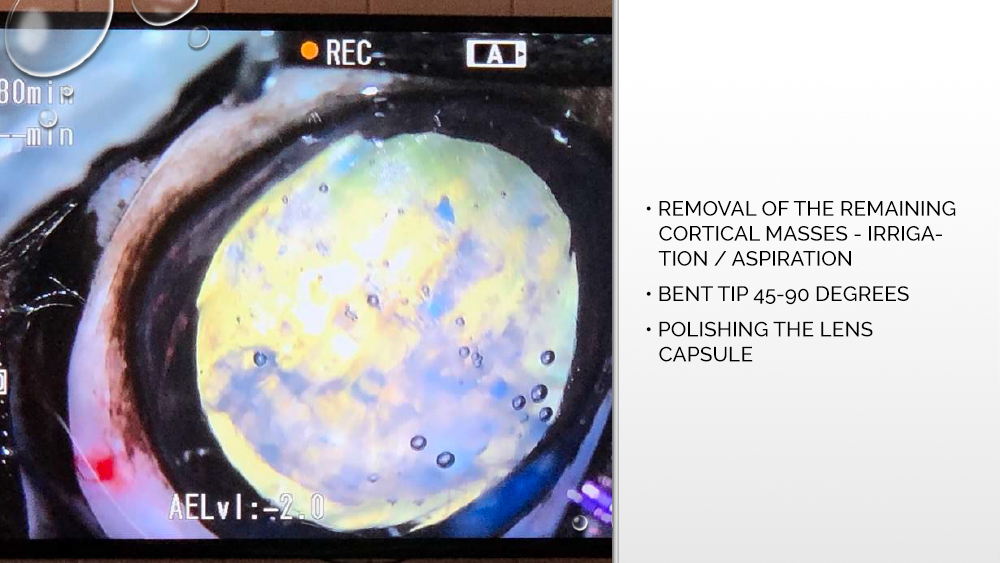
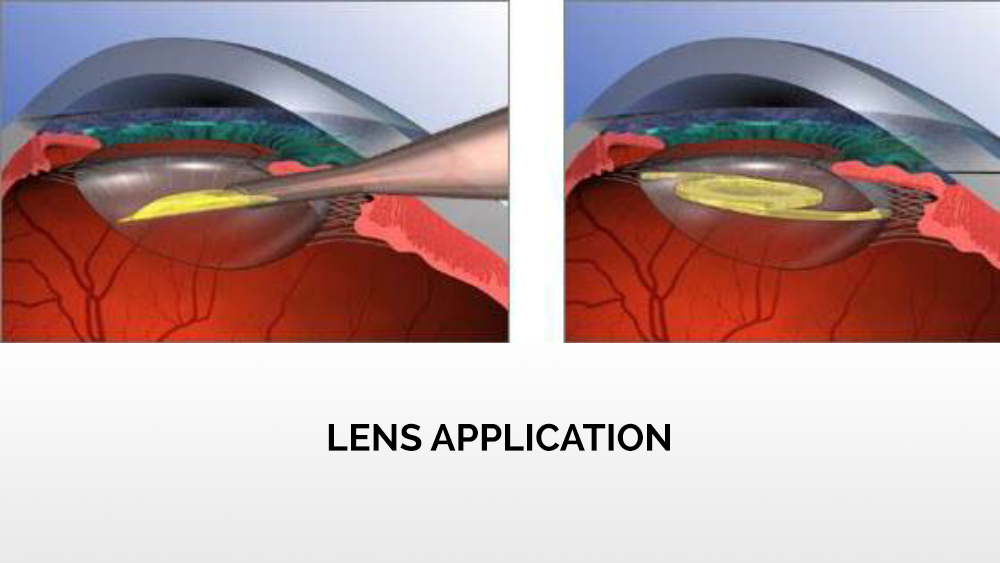
After opening, the anterior capsule of the lens is grasped and a circular, centrally positioned hole of the appropriate diameter is prepared, through which phacoemulsification will be performed, and then an artificial lens will be implanted. The tip of the phacoemulsifier is inserted into the prepared hole, which cuts the cortex of the lens and causes the formation of ultrasounds that break the cortical masses. Also using a tip, rinsing, and suctioning of the lens cortex is performed.
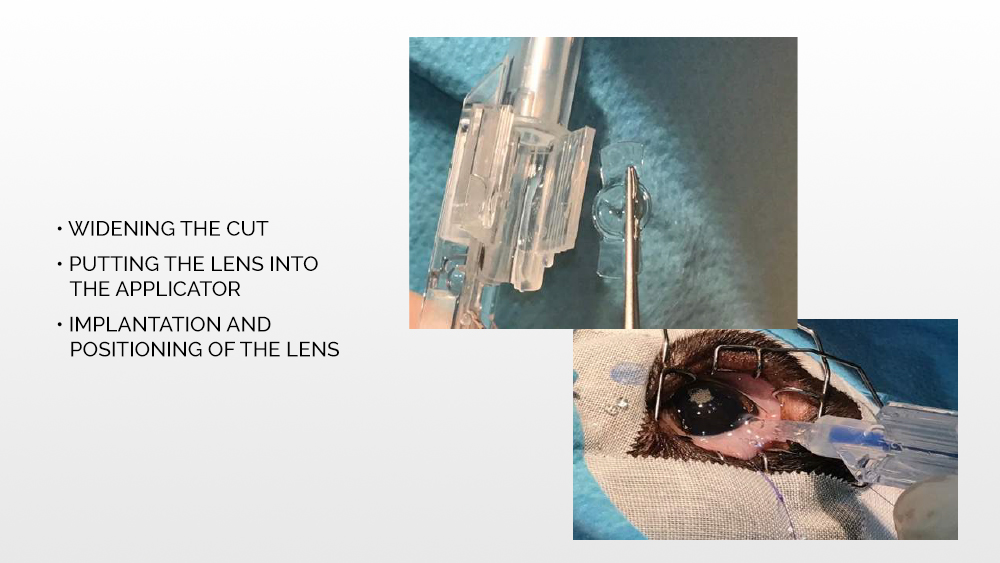
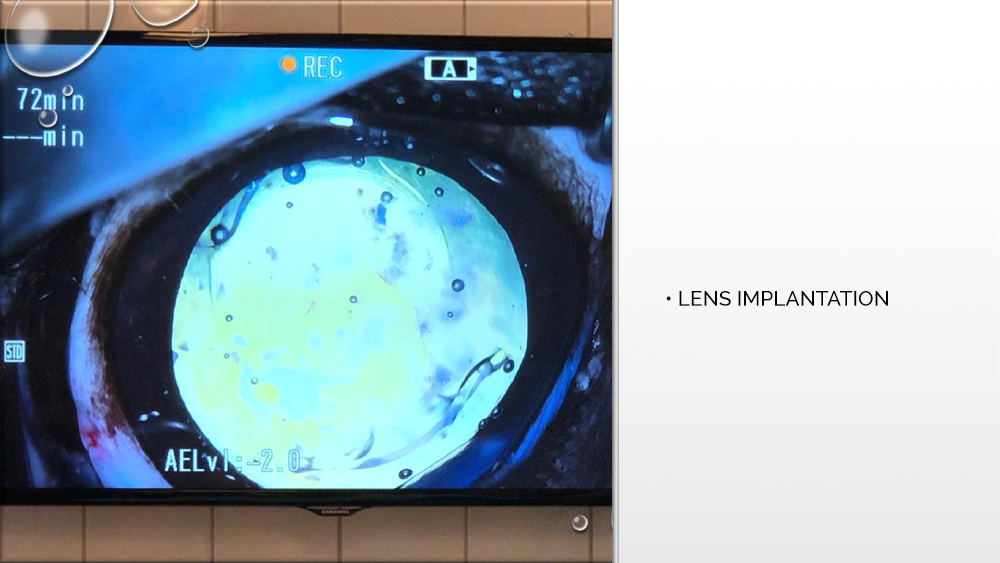
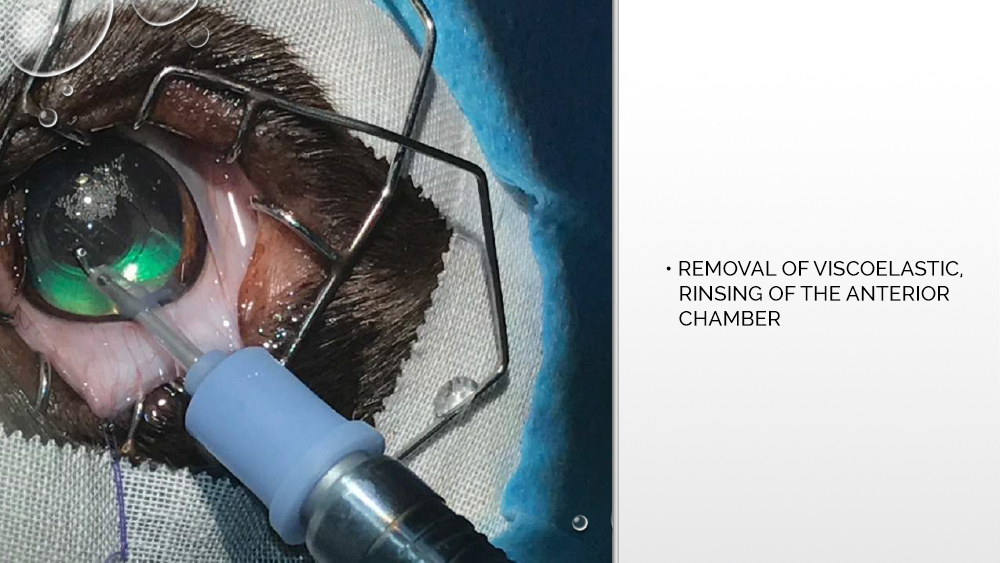
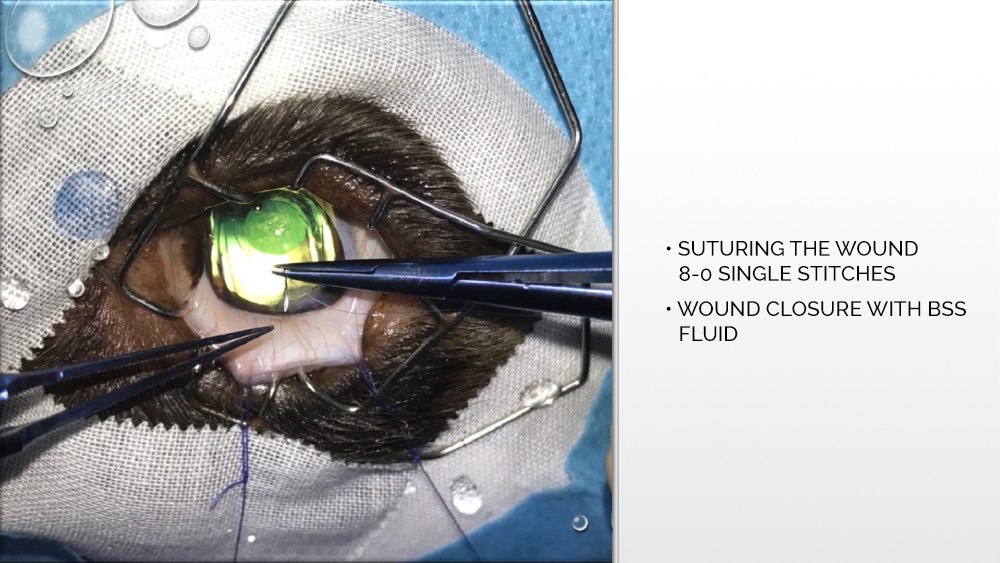
After widening the cut, an applicator with an artificial, expandable lens is inserted through the same opening through which the tip was first introduced. The lens is injected from the applicator into the eye chamber and properly positioned between the lenticular capsules. Then the viscoelastic is removed, the eye chamber is rinsed, and the wound is sutured.
See how a cataract is removed in a dog – the photos below show each of the stages of the operation.
POSSIBLE POST-OPERATIVE COMPLICATIONS
Possible postoperative complications are a topic of particular concern to owners of four-legged patients. It is reassuring, however, that the overall success of cataract surgery is estimated at just over 95%. Complications that may occur, such as discory, i.e., changing the shape of the pupil, are often only a cosmetic side effect that does not affect the quality of vision and comfort of the dog’s life.
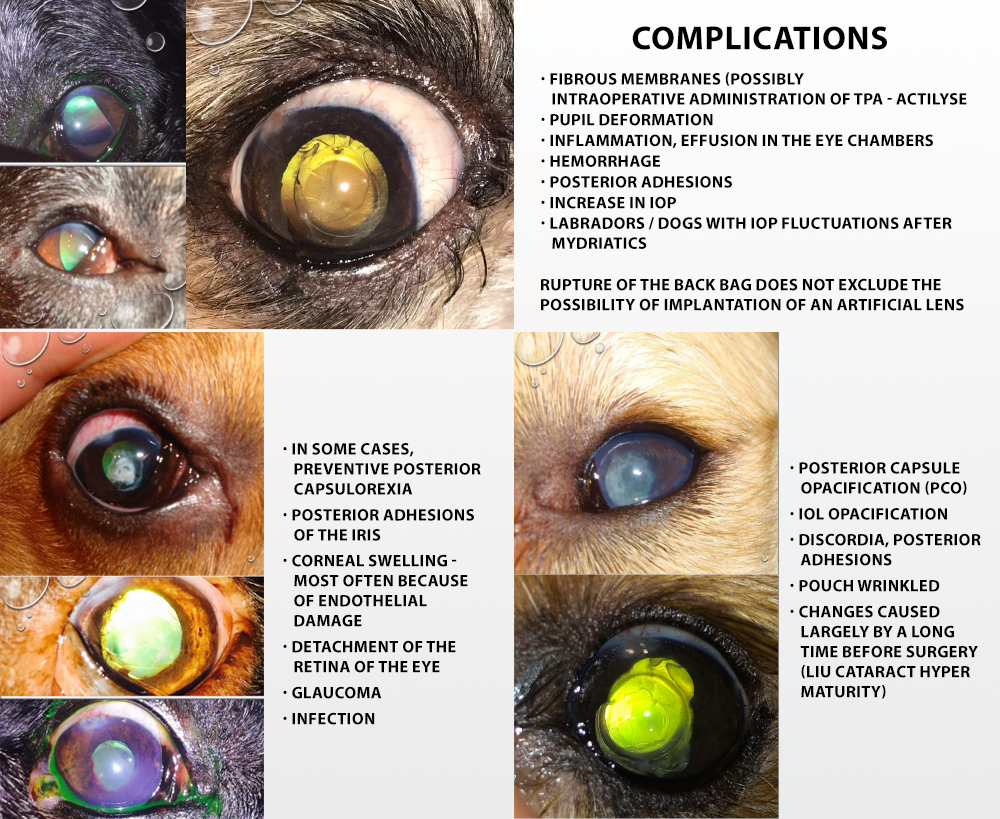
Much more serious complications that may appear after cataract surgery are, inter alia, hemorrhage (100% of cases caused by inflammation) or secondary glaucoma, i.e., fluctuations in intraocular pressure (almost 50% probability of complications in Labradors). This condition can be managed pharmacologically. The back bag may also rupture during the operation. However, if the tears are small and centrally located, the implantation procedure can be successfully continued.
In the longer period after cataract surgery, clouding of the posterior capsule may also occur, which is in fact an inevitable process that occurs to a greater or lesser extent in every patient. This is because at the equator of the cornea, irremovable cells with the ability to multiply remain. This proliferating layer of cells progresses along the posterior capsule, giving it a gradual, subtle cloudiness. In some cases, centrally located opacities appearing on the lens capsule can be removed. This procedure is called posterior capsulorexia.
After cataract surgery, the so-called cataracts may also appear in your dog. adhesions, e.g., close to the edge of an implemented artificial foldable lens. However, if the adhesions did not appear 360 ° around the pupillary edge, they did not result in any further complications. They should be prevented by taking preventive measures to dilate the pupils, the so-called mydriatic drugs.
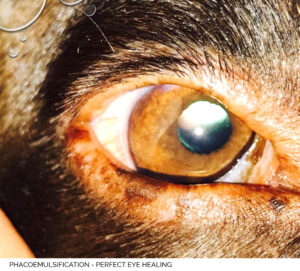
In human ophthalmology, cataract extraction is a frequent, routine procedure, providing only 0.1% of the possibility of severe postoperative complications. In veterinary medicine, the possibility of serious complications after cataract surgery is estimated at 4% -5%. This difference results from the fact that in human ophthalmology this procedure is performed much earlier than in the case of animals. The dog is unable to communicate vision problems and the owner can observe the endosperm in the dog’s eye only when they show clear symptoms, which is very late. In veterinary medicine, cataract surgery is performed in cases that would often be considered extreme in human ophthalmology. Therefore, the possibility of postoperative complications in animals is higher. It should be added that for cataracts to completely disappear in a dog, pharmacological treatment is not enough – removal is possible only by surgery. Therefore, your dog should undergo regular eye examinations for early detection of possible changes. It should also be borne in mind that, even after cataract surgery, there is still a need for regular eye check-ups.
FAQ
- What are the symptoms of cataracts in dogs?
Signs of cataract in dogs are visible spots or clouding of the lens of the eye, and deterioration in vision and behavioral changes in the quadruped. Depending on the type, the endosperm in a dog’s eye can take different shapes and occupy other areas of the eye – locally, partially, or completely, focal, or wide.
- What are the causes of cataracts in dogs?
Cataracts can be both congenital and secondary. It can occur because of mechanical injuries and inflammation of the eyeball, glaucoma, as well as metabolic diseases such as diabetes and thyroid dysfunction, or calcium deficiency, poisoning and malnutrition.
- How to treat cataracts in dogs?
The form of cataract treatment in dogs depends on the stage of the disease. The most advanced cataracts, and thus the most easily noticeable by the caregiver, can only be cured through surgery. Pharmacological therapy is used at an earlier stage of the cataract, and although it will not completely heal your pet’s eyesight, it will help slow down the progression of the disease.
Veterinarian Paweł Stefanowicz

Member of the European Veterinary Ophthalmology Association (ESVO) and the Eastern European Veterinary Ophthalmology Association (EESVO). The owner and manager of the RETINA Veterinary Clinic in Krakow, since 2006 dealing exclusively with veterinary ophthalmology.
From 2018, chairman of the PSLWMZ Ophthalmology Section. In 2008, he completed specialist training in ophthalmology at the University of Luxembourg under the ESAVS course. Participant of the ESVO (European Society of Veterinary Ophthalmology) ophthalmological congresses and the prestigious ECVO (European College of Veterinary Ophthalmologists) as well as numerous trainings and workshops in the field of veterinary ophthalmology in Poland and abroad. In 2013, he obtained the title of specialist in the field of surgery of domestic animals. In 2014, he completed an internship at the ophthalmology ward of the renowned reference specialist clinic Animal Health Trust in Newmarket, Great Britain. Author of numerous lectures, trainings, and scientific publications on ophthalmology in the professional press. One of the few veterinary ophthalmologists in Poland who perform specialized operations, such as cataract removal (phacoemulsification with implantation of artificial lenses), surgical treatment of glaucoma (gonio-implantation, trabeculectomy), cryosurgical removal of eye and appendage neoplastic lesions, and operations of the posterior segment of the eye (vitreoretinal surgery).
The host of the Pets Diag webinar: “Cataracts in dogs – causes, symptoms and treatment” (Polish version)
Our webinars in English
Do you want to know how to care for your dog’s eyesight with the help of a diet? Be sure to read:
 Feeding the dog – diet and eyesight Feeding the dog – diet and eyesight
– What else can we do to take care of our four-legged friend’s eyesight? A proper diet is also helpful.
– Which supplements should we use to take care of our dog’s eyesight? Among others, vitamins A and C, zinc, selenium, chromium, and taurine, which are nutrients that support the functions of the retina and the eye lens … |